How ICSI Works
Oocyte collection
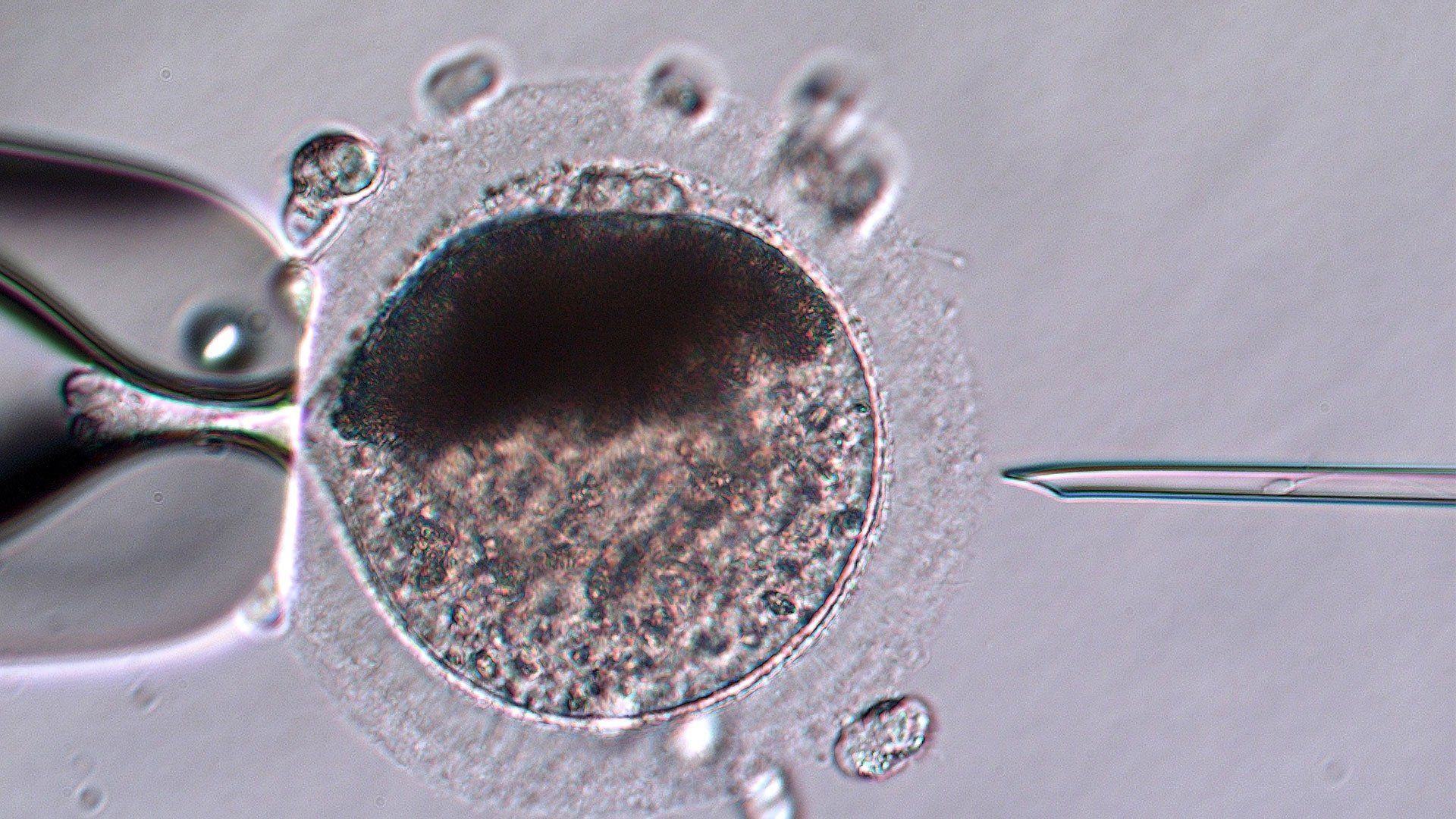
A mature oocyte positioned in preparation for Intracytoplasmic Sperm Injection (ICSI)
Oocytes (eggs) are collected from follicles on the ovaries by transvaginal follicular aspiration (TVA), also called ovum pickup (OPU). This procedure uses a double lumen needle allowing simultaneous flushing and aspiration inside the follicle. This rapid movement of fluid is necessary to dislodge the oocyte that is firmly adhered to the follicle wall in a hillock of cells – much more firmly than in most other mammals. A transvaginal ultrasound probe with a needle guide is used to visualize the follicle and guide the needle into it.
Oocytes can either be recovered just prior to ovulation from the large dominant follicle each cycle or from the smaller subordinate follicles at any time. Most commonly we collect from both the dominant and subordinate follicles at the same time each cycle. A typical mare will have one dominant and 10-12 subordinate follicles each cycle. The average oocyte collection rate is about 75% per follicle for the dominants and 60-70% for the subordinates giving an average yield of .7 oocytes from the dominant follicle and 8 from the subordinates per cycle. This is highly variable from mare to mare, as some mares have many subordinate follicles and some quite few; older mares tend to have somewhat fewer subordinate follicles. The oocyte from the dominant follicle is usually of higher quality but since the oocytes from the subordinate follicles are generally more numerous approximately 80% of the pregnancies produced come from oocytes from small follicles.
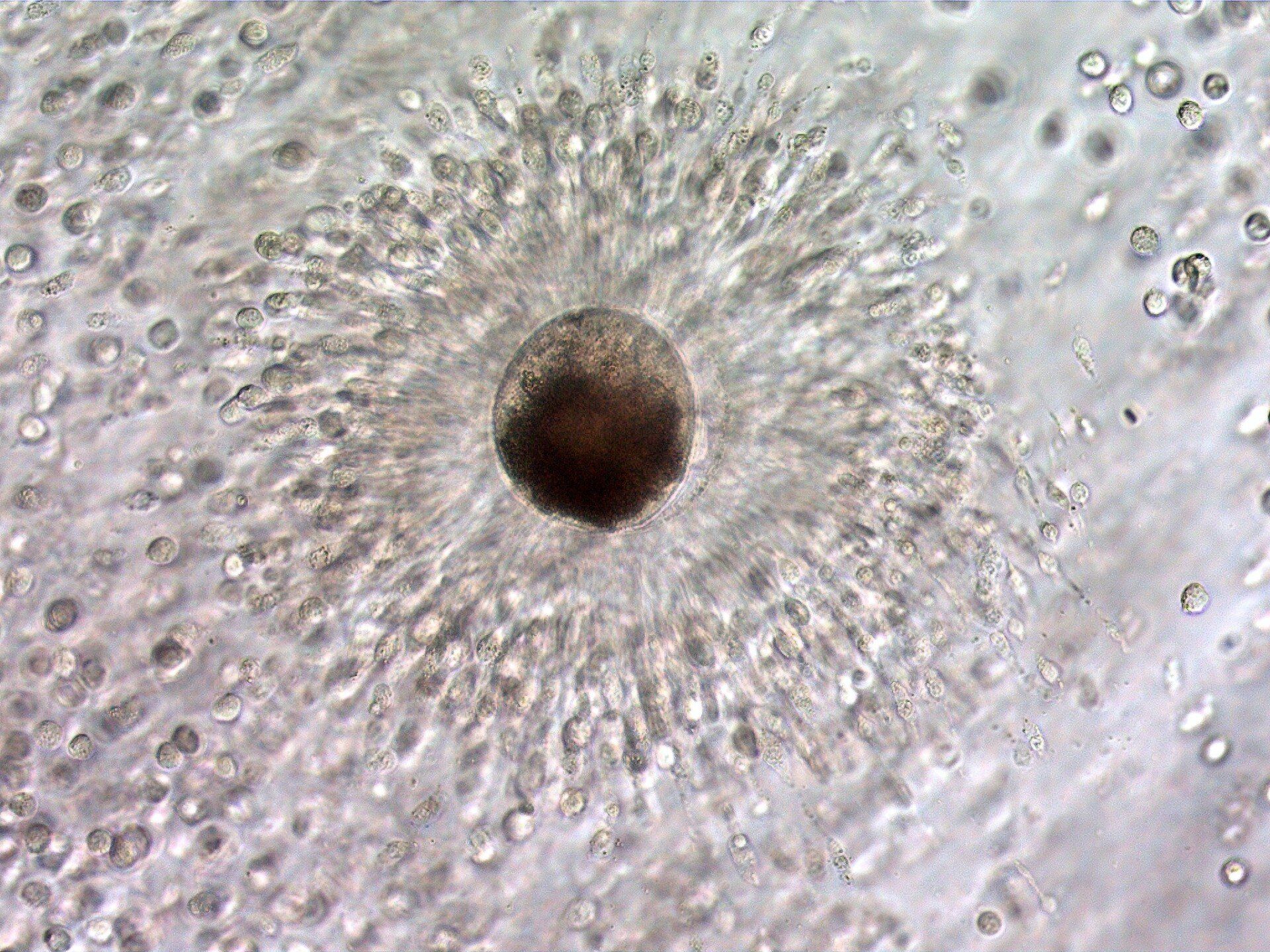
Mature oocyte in an expanded cumulus mass. The cumulus cells directly around the oocyte function to nourish the oocyte and maintain its environment, and is called the corona radiata.
Oocytes are generally recovered as a cumulus-oocyte complex, an oocyte surrounded by the cumulus cells that nourish it, dislodged from the follicle wall. Initially as a follicle grows, the cumulus cells are tightly adhered to the follicle wall and the mass of cells itself is very dense; the cells are very close together. As the follicle grows and becomes a dominant follicle the cumulus mass starts to expand as the cells secrete an extracellular matrix that spreads them apart. Nearing ovulation this expansion makes the attachment to the follicle wall weaker and weaker so that during ovulation the oocyte can be swept from the follicle into the oviduct. The loosening of the attachment makes the oocyte somewhat easier to recover nearing ovulation, although as the follicle enlarges it is more difficult to create the turbulence necessary to dislodge the oocyte. For these reasons, aspiration of the immature follicles with their firmly attached cumulus-oocyte complex, tend to have the highest recovery rate when they are between 10 and 20 mm in size, while the dominant follicles are best aspirated less than 14 or 15 hours before an expected ovulation.
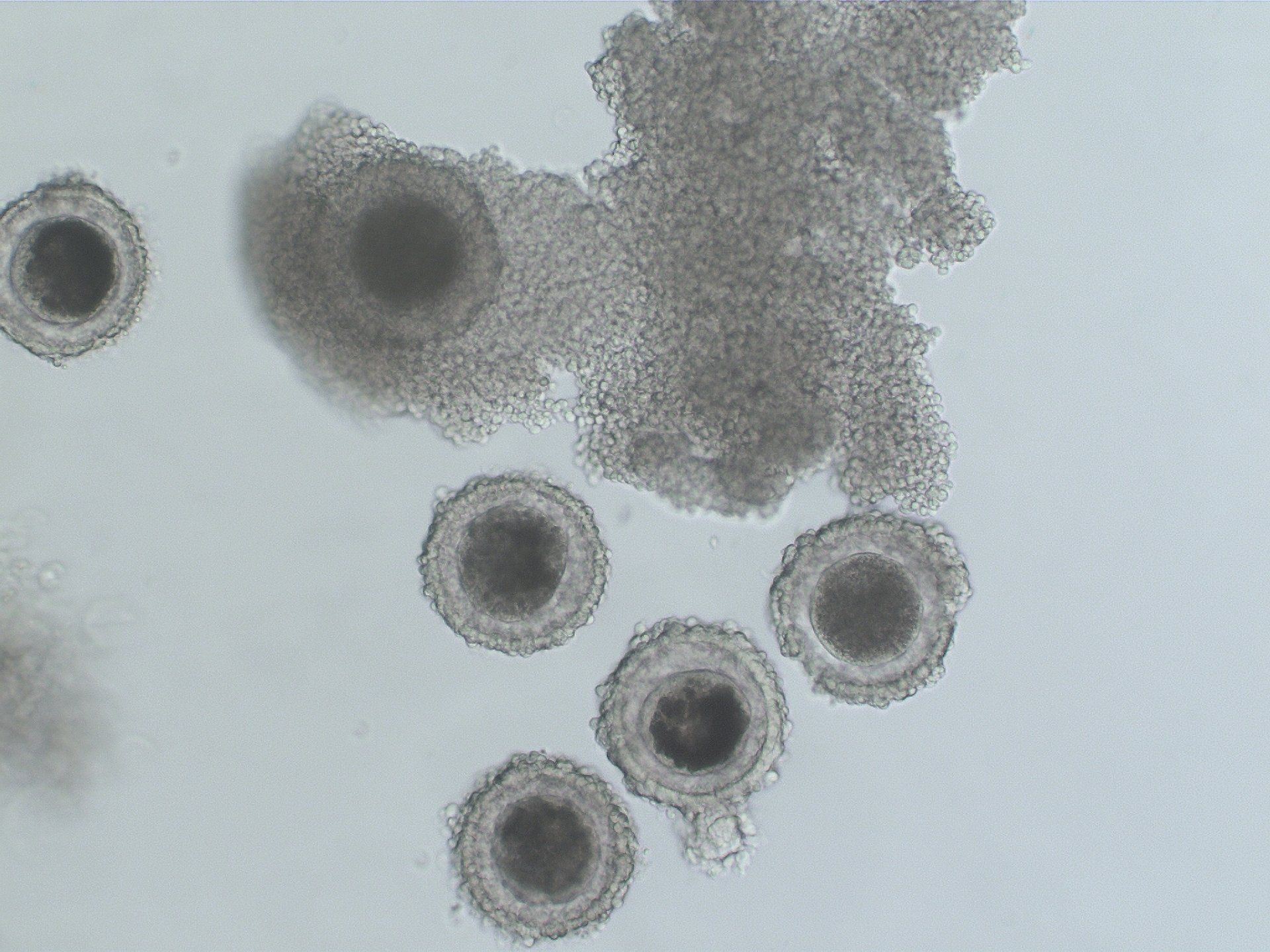
Immature oocytes collected from a single mare. The oocytes are surrounded by tight, compact cumulus cells.
When the oocytes have completed maturation (overnight for those from dominant follicles or about 2 days for those from subordinate follicles) the cumulus cells are removed to allow visualization of the oocyte for injection.
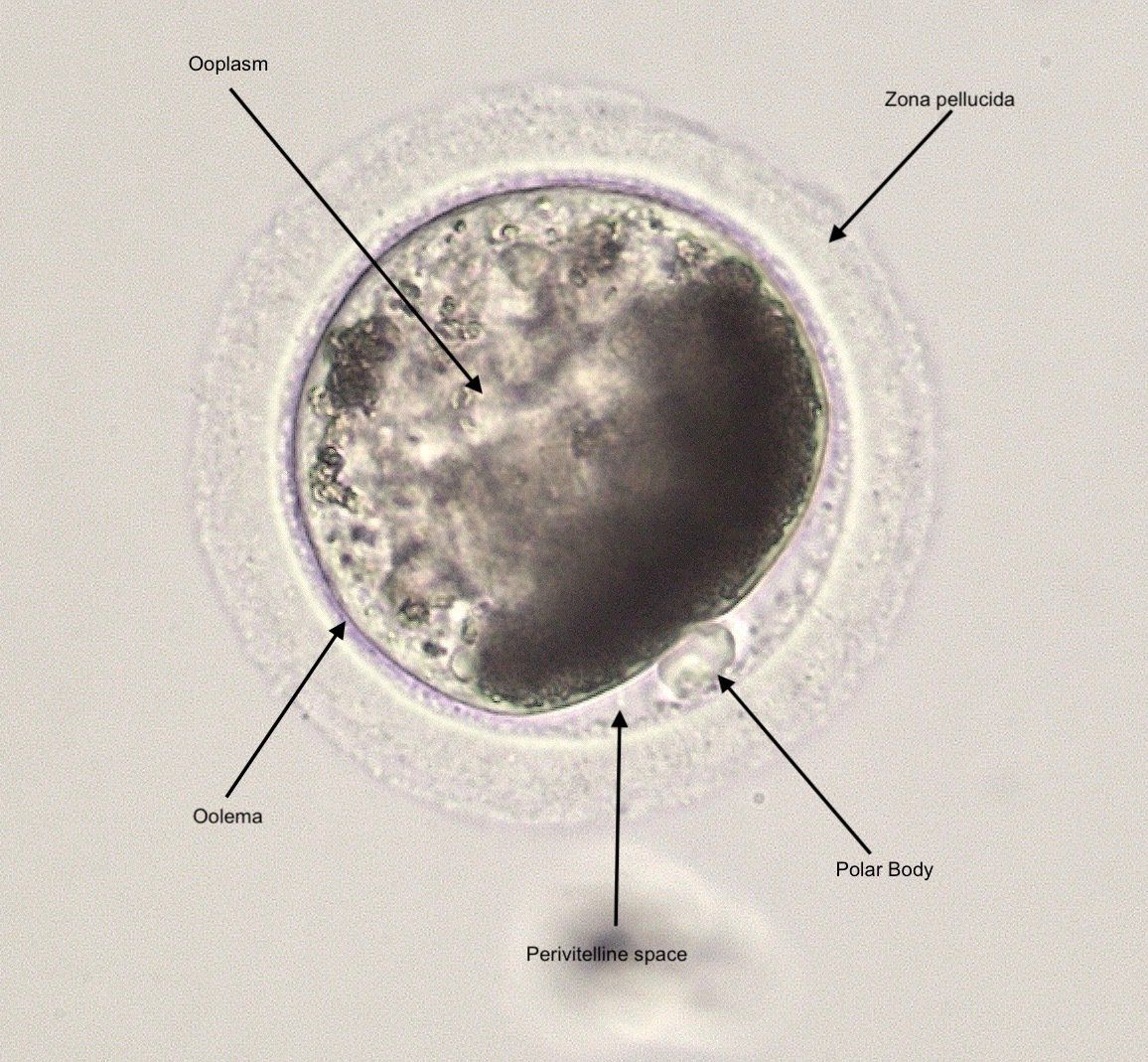
A mature oocyte at metaphase II, evidenced by the single polar body.
Sperm selection
Semen used for ICSI can be fresh, fresh-cooled, or frozen, but frozen is most commonly used. Since only a few cells are needed, generally just the tip of a frozen semen straw (about 1/10th of a straw) is cut off to thaw. This leaves the other 90% frozen to use in the future. The cells are processed in several different ways, but nearly always use a “swim-up” to help select motile cells. This is performed by placing the sperm sample at the bottom of a tube of culture medium, allowing time for the spermatozoa to swim, and the sample is taken farther up the tube.

Sperm swim-up is usually performed with a small section of a frozen semen straw that is thawed at the bottom of the swim-up medium. Motile sperm then swim up from the layer at the bottom. A sample obtained above the medium/semen interface will contain largely clean motile spermatozoa.
Individual spermatozoa are selected under the microscope and immobilized by crushing the tail with the injection pipette. Once in the oocyte, this damage to the cell membrane covering the tail will facilitate the passage of “sperm factor” into the oocyte. Sperm factor is a chemical that is critical in activating the oocyte to start the process of cell division.
Sperm Capture and Preparation Video
For the ICSI procedure itself suction on the holding pipette is used to position and stabilize the oocyte. The oocyte is positioned so that the injection will take place away from the polar body (extruded excess genetic material but near the genetic material still in the cell) and into an area of good visualization if possible.
In this video a Piezo drill is used to allow the pipette to drill through the zona pellucida and then to rupture the oolemma (the cell membrane of the oocyte).
Sperm Injection Video
Once fertilized, oocytes are placed in culture in micro-droplets under a layer of mineral oil. They are maintained in an incubator with increased carbon dioxide and decreased oxygen concentrations to regulate proper temperature, pH, and to reduce oxidative damage. The mineral oil overlay prevents evaporation of the culture medium and helps decrease the chance of contamination.

An embryo culture dish with culture medium overlaid by mineral oil.

Embryos and oocytes are cultured in an incubator that contains an atmosphere of 5% carbon dioxide to maintain culture media pH, and 5% oxygen to reduce superoxide radical formation.
When successfully fertilized and activated, an oocyte quickly starts making rapid and dramatic changes. One of the first events that can be visualized is extrusion of excess genetic material in the second polar body, often within 3-4 hours following fertilization.
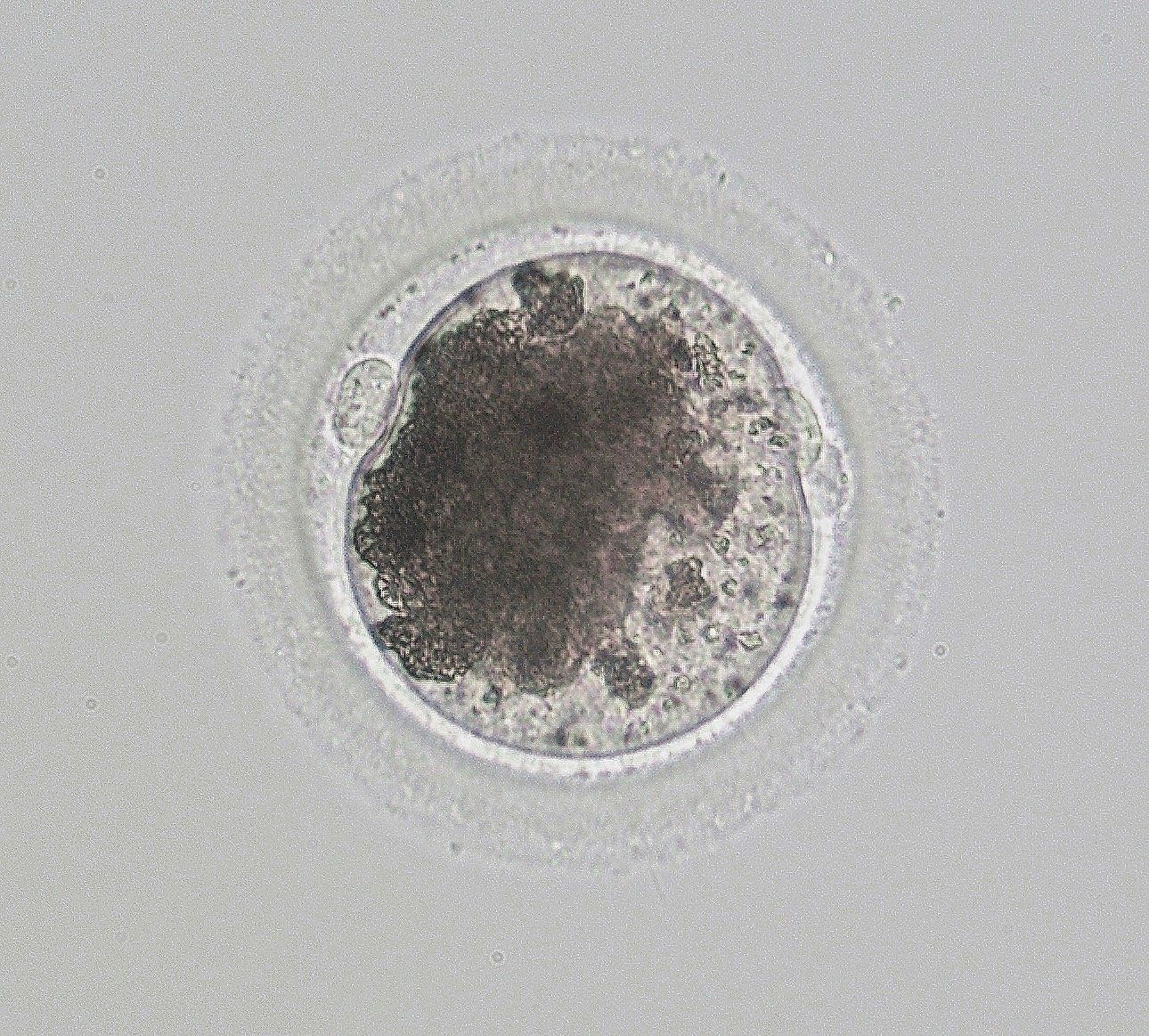
Second Polar Body Extrusion
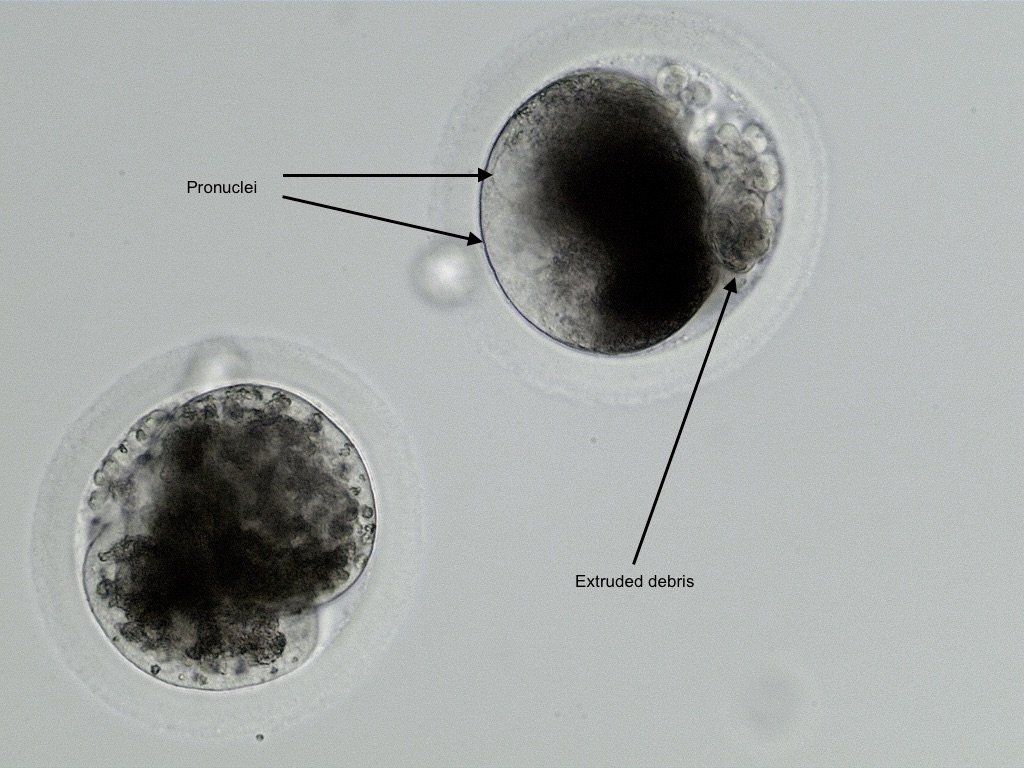
One 2 cell embryo and 1 fertilized oocyte 24 hours following fertilization. Both exhibit extruded debris commonly expelled from the oocyte a few hours prior to the first cell division. Pronuclei are sometimes visible shortly before the first division.
Approximately 70% of injected oocytes divide (cleave). The first cell division takes place within 24-30 hours. Generally the faster dividing embryos are healthier and are more likely to continue development normally. Subsequent divisions should occur approximately every 24 hours.
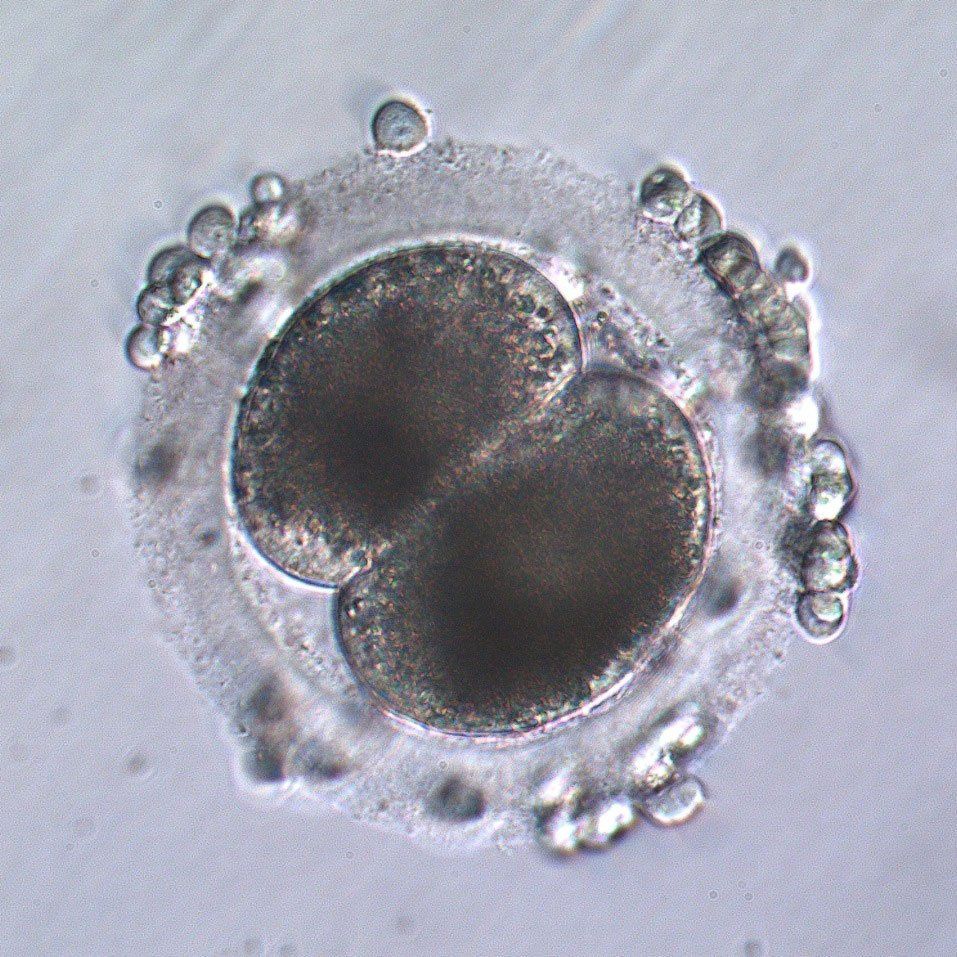
Two cell ICSI embryo, 24 hours following sperm injection. Several cumulus cells remain on the surface of the zona pellucida in this embryo.
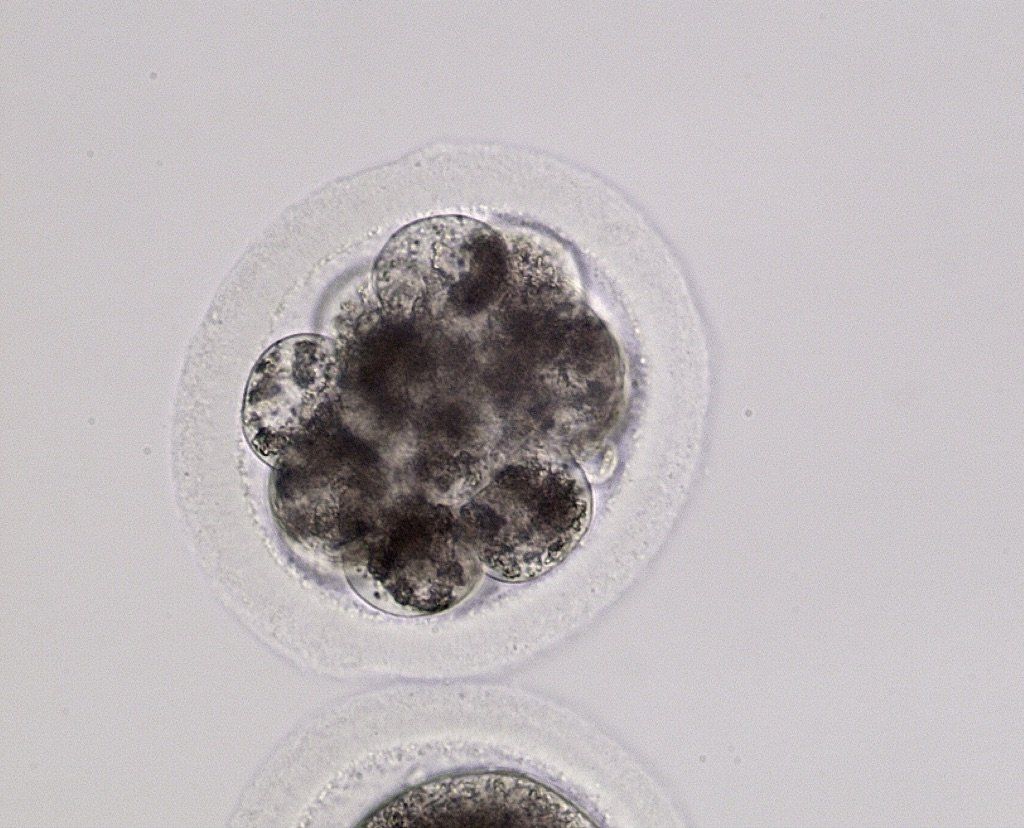
Good quality day 3 embryo.
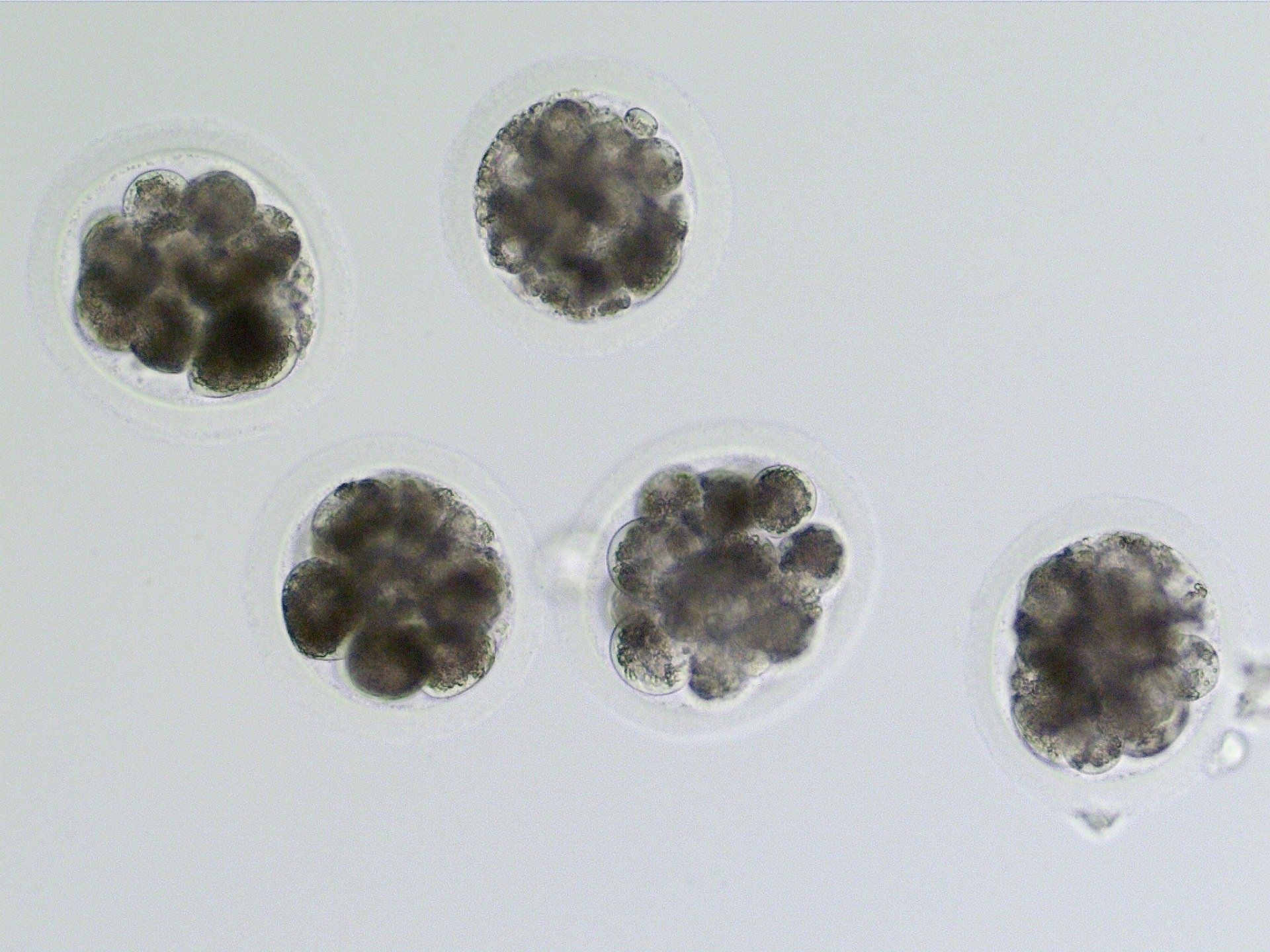
Day 4 embryos from a single mare. Only one of these embryos progressed to the blastocyst stage, was transferred, and established a pregnancy. This can be very difficult to predict early in the incubation period, as in this case where the differences in quality are not great between these embryos.
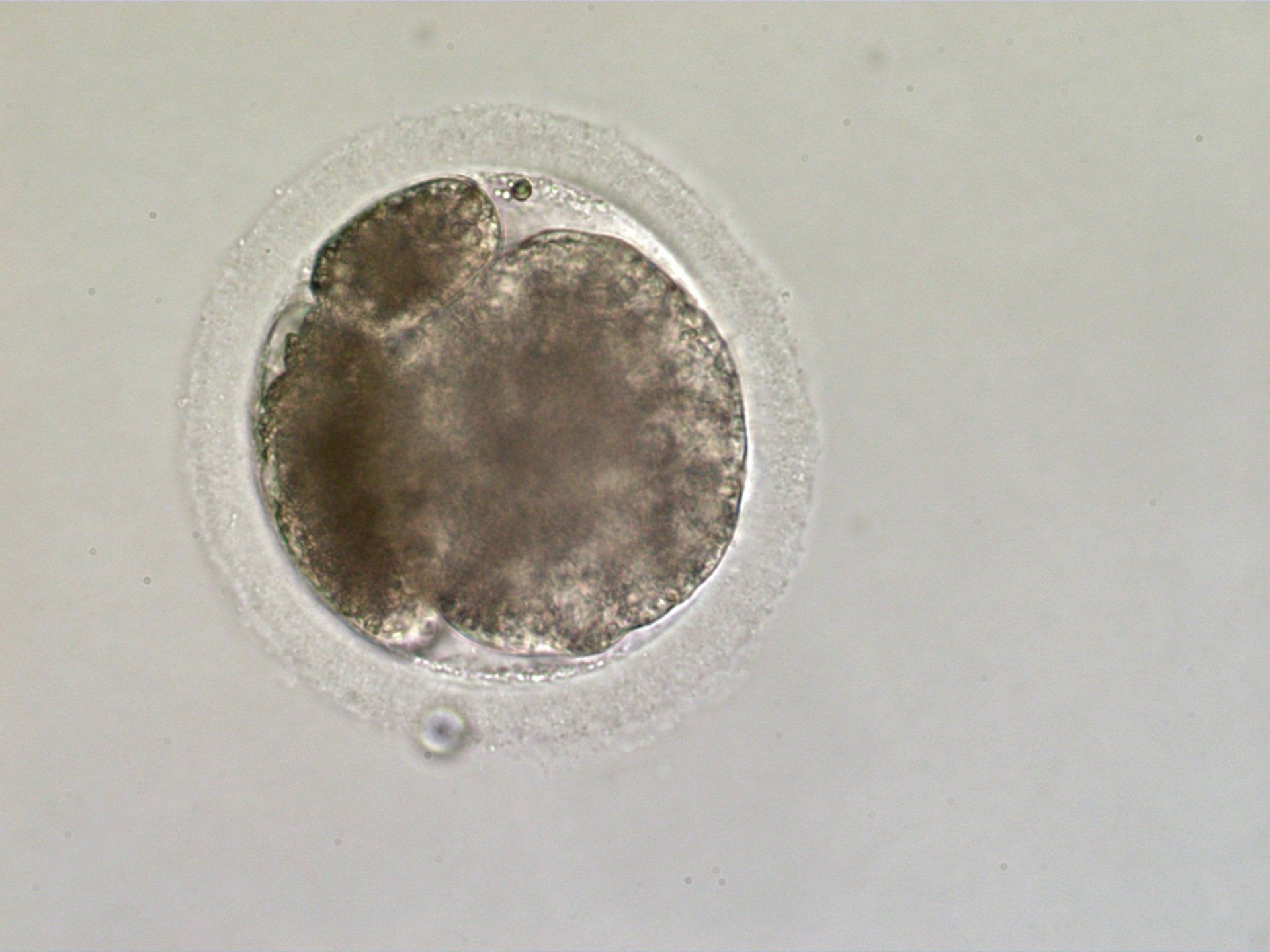
Compact morula, day 5 following ICSI. At about day 5 embryos undergo compaction where the relatively autonomous cells coalesce to become a single tissue-like mass. This is a critical step in development, many of the ICSI embryos that do not complete development arrest just prior to compaction.
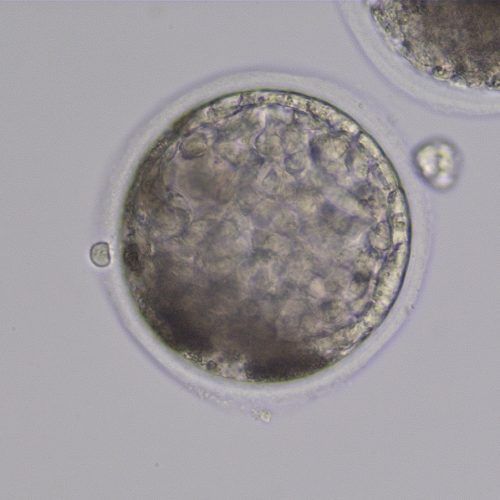
ICSI early blatocyst 7 days following ICSI. The trophoblast layer has become evident on the periphery of the blastocyst. The zona pellucida is thinning in response to the increasing diameter of the embryo. ICSI embryos tend to be a little darker than those naturally produced, and some extruded blastomeres (dead cells) can be seen between the zona and the trophoblast layer in the lower left side of this embryo.
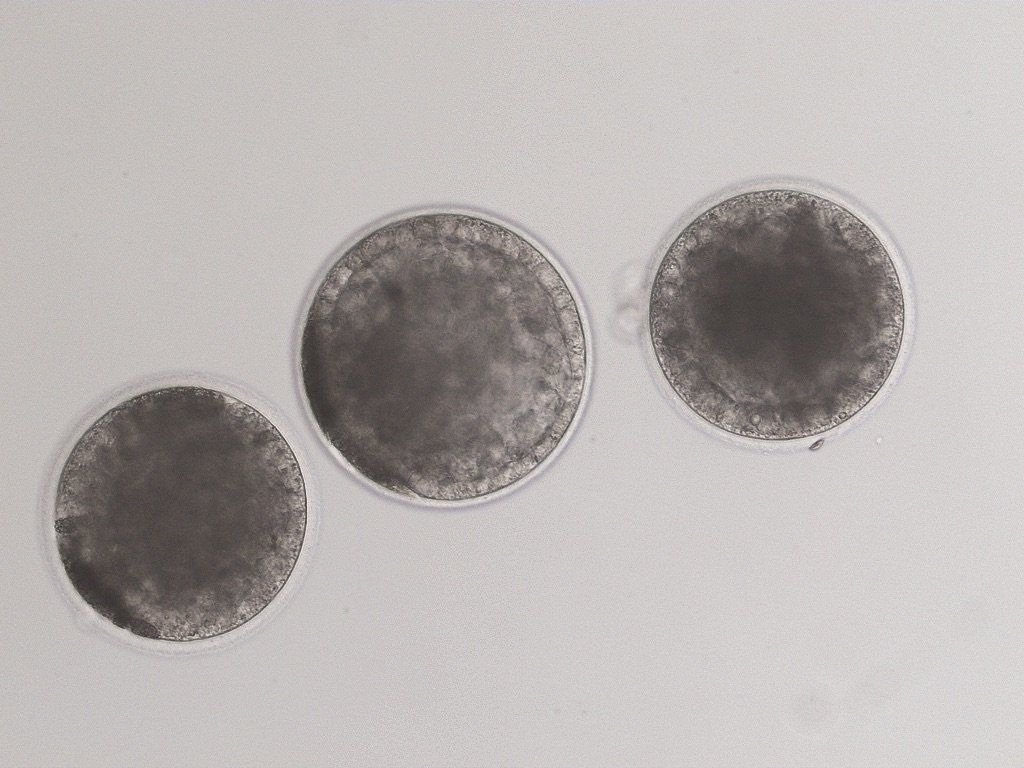
Three ICSI early blastocysts showing good trophoblast layer and the dark coloring typical of in vitro produced equine blastocysts. The trophoblast layer is very distinct on the center embryo. This is the stage ready for non-surgical embryo transfer.
Good quality ICSI produced early blastocsyts should have an approximately 80% pregnancy rate when transferred non-surgically to a recipient mare. The early embryonic loss of pregnancy is slightly higher in ICSI produced embryos than in naturally occurring pregnancies.






